Metformin, a common diabetes medication, may be associated with less development of intermediate age-related macular degeneration (AMD).

Metformin, a common diabetes medication, may be associated with less development of intermediate age-related macular degeneration (AMD).

Family-friendly format empowers continuing education.


Revisyon is described as a device-led therapy that applies specific wavelengths of low-level LED light to the crystalline lens through a non-invasive, in-clinic procedure.



A study reveals that low-dose pilocarpine effectively reduces pupil size in presbyopic eyes with minimal impact on lens thickness and accommodation.

This one-day symposium on January 31, 2026, will bring together clinicians and experts at the University Eye Clinic in Mainz to discuss optic neuropathies and diagnostic trends.

James Tsai, MD, MBA, sheds light on what is in the offing for glaucoma specialists

James Tsai, MD, MBA, discusses his approaches given the wide diversity of patients in a major urban setting when awareness of glaucoma can range from highly educated patients to uninformed individuals.

Data estimates the prevalence of glaucoma currently is almost 50% higher than previously estimated and over 1.6 million individuals in the UK are estimated to have glaucoma by 2060.

Key clinical trial data and PDUFA dates in early 2026 focus on treatments for dry eye, AMD, and rare eye diseases.
The Swiss-designed phaco platform provides mobility, simplified workflows, and reduced surgical waste for cataract procedures, according to the company.
Patients underwent a full ophthalmologic examination that included optical coherence tomography (OCT), OCT angiography, and biometry.

“Remarkable” results were reportedly obtained with hypotony with hydroxypropyl methylcellulose.

Optoretinography is an emerging technology used to test light-evoked photoreceptor activity.
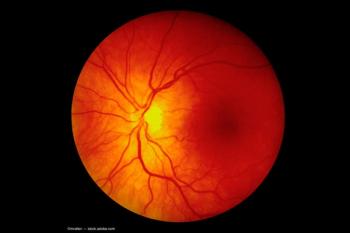

Researchers uncover a DNA repair mechanism in Greenland sharks that preserves their vision for centuries, offering insights into longevity and eye health.
A recent study reveals significant ocular complications from monkeypox, highlighting the need for enhanced eye health strategies in affected regions.
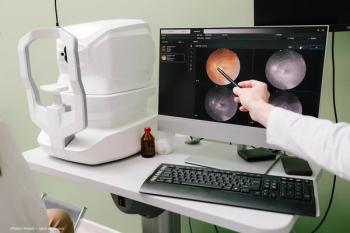
A recent study represents a step forward in investigations of the retinal layers as they are affected by glaucoma.

The letter noted the FDA is unable to approve the application for ONS-5010/LYTENAVA (bevacizumab-vikg) in its current form for the treatment of wet AMD, according to the company.
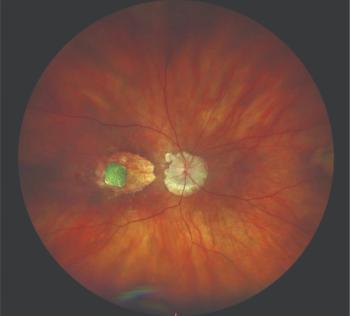
The novel system converts light into electrical signals to stimulate retinal cells.
Strategies for treatment intervals, drug selection, and patient expectations.


Panel examines drug mechanisms, patient factors, and strategies to optimize results.



Published: February 24th 2025 | Updated: March 10th 2025

Published: May 15th 2024 | Updated: May 20th 2024

Published: August 25th 2023 | Updated:

Published: July 9th 2022 | Updated:

Published: April 23rd 2025 | Updated:
Published: April 6th 2024 | Updated: